Fitness and The Lymphatic System: An Overview
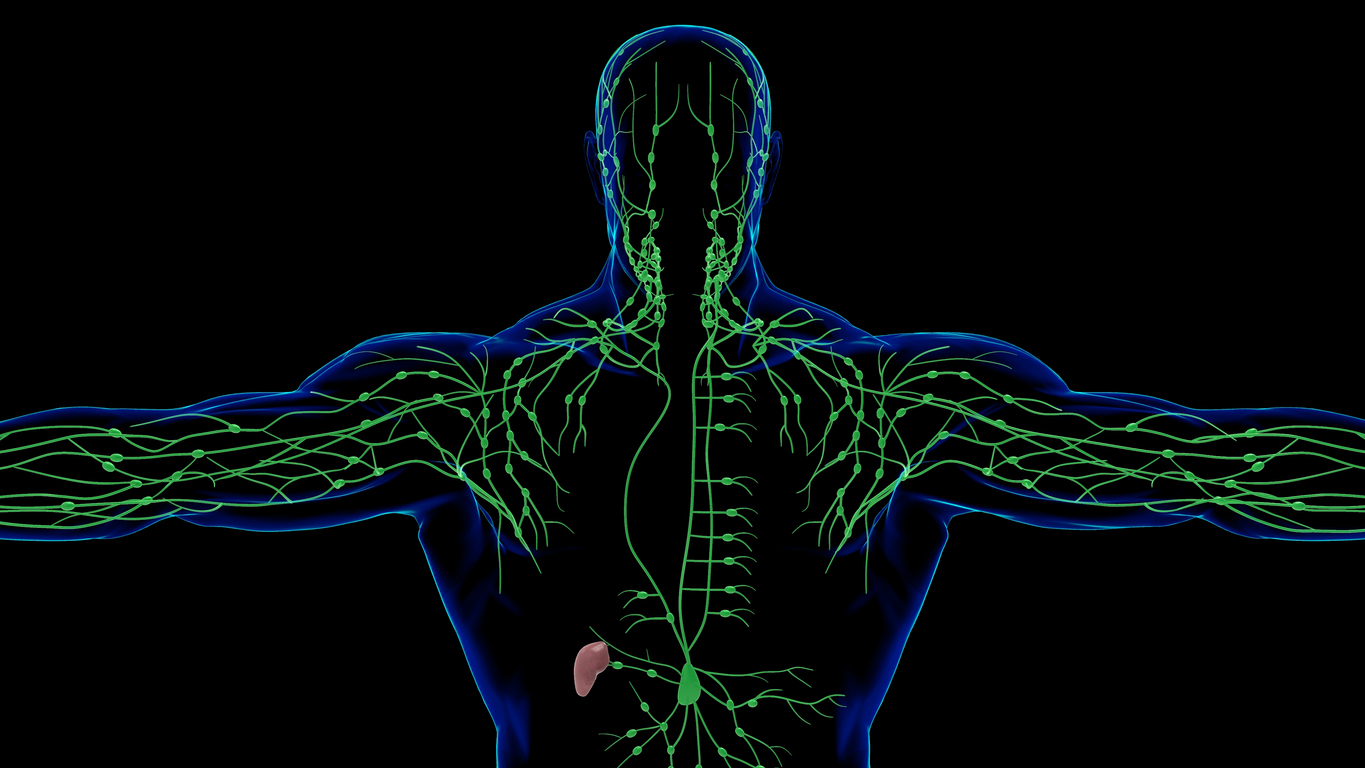
The lymphatic system is an important component of the circulatory, immune, and metabolic systems and is comprised of lymphatic fluid, lymphatic vessels, and lymphatic cells, including macrophages, dendritic cells, lymphocytes, and the lymphatic organs, such as the spleen and thymus (Ozdowski & Gupta, 2022). This system acts as a web of highways that transport waste and junk out of the body and has a multitude of other functions; however, some of the most important roles encompass the regulation of tissue pressure, immune surveillance, and the absorption of dietary fat. Additionally, there is substantial evidence to suggest that the lymphatic system contributes to the development of diseases, such as lymphedema, cancer metastasis, and several inflammatory disorders (Cueni & Detmar, 2008). Therefore, any disruption to this system can have catastrophic effects on the human body.
Health, disease, and the lymphatic system are terms frequently observed together in the wellness industry. The lymph nodes provide a highly sophisticated microarchitecture that supports optimal surveillance of the immune system, with disruptions to this organized framework compromising immune function and resulting in lymphedema (Liao & Padera, 2013). Other conditions tied to the lymphatic vasculature include lymph accumulation in tissues, dampened immune response, and the accumulation of tissue and fat (Alitalo, 2011).
The relationship between fitness and the lymphatic system has been widely established in the healthcare industry. Many systems within the human body rely on physical activity to function, and the lymphatic system is no exception to this. Exercise not only gets your muscles moving and increases your heart rate, but it also stimulates lymphatic flow. The lymphatic system relies mainly on gravity and muscle contractions to allow for it to function properly, and without movement, the necessary pumping action is non-existent. In turn, this has been hypothesized to encourage the lymphatic system to function more efficiently and potentially prevent infections and other diseases from arising in the body (Lane et al., 2005). The lymphatic system also functions optimally when you are at a healthy weight, highlighting the importance of fitness. Several recent studies have provided evidence to suggest the relationship between obesity and impaired lymphatic function, from the accumulation of inflammatory cells around lymphatic vessels to alterations to the gene expression of lymphatic endothelial cells (Kataru et al., 2020).
A 2016 study by Hespe et al. investigated the relationship between exercise training and obesity-related lymphatic dysfunction. Participants were randomized to either aerobic exercise or a sedentary group that were not permitted to conduct physical activity during the study period, with lymphatic function analyzed prior to the study and after six weeks. The findings demonstrated that sedentary participants had a notable decrease in several lymphatic measures, including collecting lymphatic vessel pumping capacity, lymphatic vessel density, and the lymphatic migration of immune cells. Moreover, there was a marked increase in lymphatic vessel leakiness when compared to those who undertook regular physical activity during the six week period. Although not causing significant weight loss, aerobic exercise resulted in a substantial improvement in lymphatic function (Hespe et al., 2016). These findings show that obesity impairs the function of the lymphatic system via several mechanisms and that regular aerobic exercise can function to reverse these pathological changes.
Another study was conducted in sheep and found that in those “with intact lymphatic system, undergoing short duration exercises, there was a higher frequency of lymphatic vessel contractions and lymph flow” (McGeown et al., 1987; Oliveira et al., 2018). The underlying mechanism of this improved lymphatic flow results from the increased blood pressure and cardiac output that occurs following exercise. This leads to an increase in capillary filtration and interstitial pressure. Collectively, this permits and facilitates the entry of both fluid and proteins into the lymph capillaries (Oliveira et al., 2018). As described by a 2005 Sports Medicine review, “regardless of what happens to the lymphatic vessels, the positive impact of exercise on the muscle and cardiovascular systems seems to favor the removal and circulation” (Lane et al., 2005).
When fitness is ignored, the lymphatic system is affected. The relationship between the lymphatic system and physical activity has been discussed on a large scale in recent years, given the growing prevalence of obesity. The available data demonstrates that the impact of poor fitness extends beyond aesthetics, with the lymphatic system often becoming impaired, resulting in increased inflammation, the development of disease, and altered gene expression of lymphatic endothelial cells. Most movement, whether that is walking, running, swimming, rebounding on a mini-trampoline, yoga, resistance training or playing sports can stimulate your lymphatic system, while lack of activity and prolonged sitting will promote more toxins and waste accumulation which can lead to downstream disease.
Dan Tatro-M.S.-CSCS
CEO – OC FITNESS COACH
REFERENCES
Alitalo, K. (2011). The lymphatic vasculature in disease. Nat Med, 17(11), 1371-1380. https://doi.org/10.1038/nm.2545
Cueni, L. N., & Detmar, M. (2008). The lymphatic system in health and disease. Lymphat Res Biol, 6(3-4), 109-122. https://doi.org/10.1089/lrb.2008.1008
Hespe, G. E., Kataru, R. P., Savetsky, I. L., García Nores, G. D., Torrisi, J. S., Nitti, M. D., Gardenier, J. C., Zhou, J., Yu, J. Z., Jones, L. W., & Mehrara, B. J. (2016). Exercise training improves obesity-related lymphatic dysfunction. J Physiol, 594(15), 4267-4282. https://doi.org/10.1113/jp271757
Kataru, R. P., Park, H. J., Baik, J. E., Li, C., Shin, J., & Mehrara, B. J. (2020). Regulation of Lymphatic Function in Obesity. Front Physiol, 11, 459. https://doi.org/10.3389/fphys.2020.00459
Lane, K., Worsley, D., & McKenzie, D. (2005). Exercise and the lymphatic system: implications for breast-cancer survivors. Sports Med, 35(6), 461-471. https://doi.org/10.2165/00007256-200535060-00001
Liao, S., & Padera, T. P. (2013). Lymphatic function and immune regulation in health and disease. Lymphat Res Biol, 11(3), 136-143. https://doi.org/10.1089/lrb.2013.0012
McGeown, J. G., McHale, N. G., & Thornbury, K. D. (1987). The role of external compression and movement in lymph propulsion in the sheep hind limb. J Physiol, 387, 83-93. https://doi.org/10.1113/jphysiol.1987.sp016564
Oliveira, M. M. F., Gurgel, M. S. C., Amorim, B. J., Ramos, C. D., Derchain, S., Furlan-Santos, N., Dos Santos, C. C., & Sarian, L. O. (2018). Long term effects of manual lymphatic drainage and active exercises on physical morbidities, lymphoscintigraphy parameters and lymphedema formation in patients operated due to breast cancer: A clinical trial. PLoS One, 13(1), e0189176. https://doi.org/10.1371/journal.pone.0189176
Ozdowski, L., & Gupta, V. (2022). Physiology, Lymphatic System. In StatPearls. StatPearls Publishing



